SANITATION
By Jeffrey L. Kornacki, Ph.D.
How and Why Environmental Monitoring Programs Add to the Bottom Line
A new way to see the business value in commitment to food safety

Photo credit: GCShutter/E+ via Getty Images
Over three decades of active consultation with the food industry, largely on microbiological matters related to investigation, risk assessment, and control, I have seen companies in both the best of times and the worst of times. During hundreds of visits to many food processing companies, I sometimes get the impression that food safety programs and environmental monitoring programs (EMPs) are unwanted necessities to prevent recalls or meet a requirement of regulators or customers. The basic presumption in these instances is that such programs drain profits because of sampling, testing, personnel, and other costs. My contention is that quality assurance and food safety programs, including EMPs, done well can add to the bottom line of food processors.
In all of life, the idea of perfection and the actual reality of a situation often create frustration, dissonance, and sometimes resignation as one realizes that he or she fell short of some previously undefined goal. The phrase “Well, that’s the way it is,” as well as the song “Slip Slidin’ Away,” comes to mind. However, perfection is in the eye of the beholder, and if left undefined, it can mean anything at any time. Vague concepts like “good quality” and “goodness” mean different things to different people. But if a requirement is defined narrowly and precisely, it can be achieved most of the time. For example, we expect that we will receive exact change when we purchase something. It is a known requirement of society. This rarely fails. Society is intolerant of “approximate” change. We need, as food industry and quality assurance professionals, to move beyond vague concepts of perfection and good quality and carefully define our achievable criteria, wherein deviation is not tolerated. These are our requirements. The difference between the cost associated with nonconformance and the requirements results in “the price of nonconformance” or PONC. PONC is the measure of quality.¹ As such, it can be measured in dollars subtracted from the bottom line.
Examples of the PONC
The following are examples of the PONC associated with presence of pathogens, spoilage organisms, and indicator organism findings.
Pathogens
The most dramatic PONC, the presence of a pathogen in a food, results in a series of PONCs. These can include the costs associated with illness or death, government investigations [e.g., Department of Justice, U.S. Food and Drug Administration (FDA), U.S. Department of Agriculture, state and local regulators], damage to a company’s reputation (particularly in the case of a product recall or foodborne illness) leading to loss of market share, production line shutdowns to find sources of contamination, internal investigations and testing, as well as those associated with repairing and replacing equipment and facility structures in response to finding contaminated sites. Also included are the costs of remanufacturing and replacing contaminated product with uncontaminated product (provided one still has the previously affected clients), class-action suits launched by stricken consumers and those who thought they were stricken, the costs associated with revising Hazard Analysis and Risk-Based Preventive Controls (HARPC), insurance claims, and the cost of litigation and fines.
Spoilage Organisms and Shelf Life
It often occurs that, even if spoiled product does not contain a pathogen, sometimes individuals who eat the product claim illness anyway, resulting from a perception that it is unsafe. This can result in allegations of illness, unnecessary lawsuits, and most of the other issues listed above, except in the cases of company revisions of their HARPC and resultant criminal investigations that may result from foodborne illness and death.
Shortening of shelf life due to spoilage can result in the PONC of loss of market share, but lengthening of shelf life can mean greater distribution and greater market share and company profitability. Even spoiled product can result in regulatory actions.
Out-of-Specification Contamination with Indicators
Products with out-of-specification indicator organisms can result in rejection of product, costs associated with remanufacturing product, investigations, testing costs, and many of the other issues previously described.
How EMPs for Pathogens Relate to Spoilage and Out-of-Specification Product Results
The industry’s requirement under law is to produce safe and unadulterated food, as described in 21 C.F.R 117, “Current Good Manufacturing Practice, Hazard Analysis, and Risk-Based Preventive Controls for Human Food.” For example, it is utterly unacceptable to produce a food contaminated with a low-dose pathogen, like Salmonella or Listeria monocytogenes, or a virulent Shiga toxin-producing strain of Escherichia coli (STEC).
A correlation between Listeria spp. in the environment (floors) and equipment has been demonstrated in various studies.²⁻⁴
Furthermore, Thimothe et al.⁵ showed a significant (P < 0.0001) correlation of environmental L. monocytogenes to finished product in a cold smoked fish product. It is likely that these same principles apply to other pathogens, indicators, and spoilage organisms.⁴
This highlights the rationale for a good EMP in one’s facility. In the Code of Federal Regulations [21 C.F.R. 117.165(3)], FDA requires “...environmental monitoring, for an environmental pathogen or for an appropriate indicator organism, if contamination of a ready-to-eat food with an environmental pathogen is a hazard requiring a preventive control, by collecting and testing environmental samples….” The purpose of this approach is to verify that appropriate sanitation preventive controls are being applied in the plant.
“We need…to move beyond vague concepts of perfection and good quality and carefully define our achievable criteria, wherein deviation is not tolerated.”

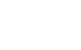
Economic Gains of Effective EMPs
The actions that control vegetative pathogens like Listeria, Salmonella, or STEC will also control vegetative spoilage and indicator organisms, resulting in reduction of the PONC. The result is that an effective EMP will result in cost savings. Costs saved are profits gained, as illustrated in Figure 1.
FIGURE 1. Relationship of EMP Results (A) and Profits (B) to the PONC
Other Items to Include in Effective EMPs
In my view, vector sample approaches should be a plant’s first attempt to determine how a particular site became contaminated. Such approaches should be more than a box that is checked. If an adequate reason cannot be found for why a location tested positive or why the vector samples tested positive, then further investigation should be done if the goal is true control of the organism. The idea is to consider how the site may have become positive. Such approaches should go beyond just sampling within a circle or starburst pattern but include determination of traffic patterns (both human and wheeled vehicles), airflow, potential for roof leaks, presence of untrapped drains, dust, or product accumulations on overheads, unhygienically designed equipment or poorly designed air-handling systems,⁶ among others. Testing for indicators like the hydrogen-sulfide-producing thermoduric Enterobacteriaceae (HTEB) indicator assay or hygienic quality assay (HQA) in place of Salmonella or Listeria, respectively, should be considered for those samples with product contact implications.⁴ Approaches to source tracking such as isolate ribotyping or phenotype biotyping can be considered to identify sources. However, applications like whole-genome sequencing are fraught with many nuances and that, as well as these other approaches, should not be attempted apart from appropriate consideration of all implications of such testing.⁷
Documented Corrective Actions
Failure to document the effectiveness of corrective actions taken in response to a positive pathogen or indicator finding is merely documentation of an unacceptable event. However, documentation of the corrective action followed by several negative sponge/swab samples (usually three consecutive samples across several days or cleaning cycles) is taken as verification of the efficacy of those corrective actions.⁸ Therefore, many EMPs have a requirement for three consecutive negative swab events.
Tracking and Trending
Sites sampled should be mapped, and the maps should indicate the presence of both positive and negative findings. A review of positive sites should be done at some frequency.⁸ For example, a pathogen finding only a few times a year at the same site may indicate a deeper problem than merely a failure to clean or sanitize.
Annual Aggressive Sampling (“Swab-a-Thons”)
The microbial ecology in a food processing environment is highly dynamic. What was a relevant EMP a year ago might not be relevant today. Microorganisms can be persistent in areas overlooked in routine sampling programs.⁹
Therefore, at least once per year, an extensive and aggressive zone 2–4 sampling of the plant environment should be done, unless a compelling reason can be identified for not doing so. This approach could be combined with a risk assessment approach.⁴ The results of this annual sampling should be used to recalibrate the EMP. Environmental sampling is typically like peeling an onion. During these high-intensity annual environmental sampling events, plants may wish to sample “basic care” areas that are typically overlooked in such programs. All too often, there is inadequate thought given to appropriate separation of hygienic zoning such as described by Chen et al.¹⁰ However, microbes are highly adaptive, and perfect control of their transmission from area to area should not be expected. This is consistent with FDA’s Listeria Draft Guidance,¹¹ where, regarding Listeria spp., it states, “If you consistently see negative test results in environmental samples collected from your plant, we recommend that you revise your environmental monitoring procedures to add, substitute, or both add and substitute other surfaces in your plant for sample collection and testing to ensure you are not missing a source of contamination.” Hence, there is an ongoing need to be appropriately diligent in our environmental sampling and vectoring and corrective action programs.
“…an effective EMP will result in cost savings.”

The Missing Link: Zone 1 and Product Testing Approaches
EMPs typically ignore zone 1 sampling. The usual rational is that such areas are readily cleaned, until one considers the FDA philosophy that these can be areas where contaminants can “drip, drop, or slough” into the product contact surface during operations. This is illustrated in the FDA approach to zone 1 testing in their Listeria Draft Guidance,¹¹ where it is recognized that contamination on a product contact surface can be discharged from areas close to product over time as opposed to pre-operationally (e.g., post-sanitation). A few examples of this could be a contaminated bearing directly adjacent to product on a conveyor, non-hermetically sealed hollow rollers for product contact surfaces of belts, and gaskets on flanges for rotary valves,³ wherein moisture has accumulated, etc. Pathogen testing on such zone 1 surfaces is generally discouraged. Hygienic indicators are often employed for testing such surfaces and are the principal reason why the HTEB indicator assay and HQA were developed.⁴
Companies employing finished-product pathogen or indicator testing should consider increasing or decreasing statistical sampling of product in response to increases or decreases in microbiological findings in the environment based upon proximity to product.
Conclusion
Costs associated with EMPs may be perceived as subtracting from a company’s bottom line. However, given the PONC associated with product contamination from pathogens, spoilage organisms, and indicators, appropriate corrective actions taken in response to a robust EMP can add to the bottom line. Food companies are encouraged to develop appropriate metrics to determine correlations between reductions in pathogens and indicator organisms in their routine (noninvestigatory) EMPs and reductions in the PONC and therefore increase profitability while simultaneously reducing public health risk.
References
1. Crosby, P., Quality Without Tears: The Art of Hassle-Free Management (New York: McGraw-Hill, 1995).
2. Tomkin, R.B., et al. 1992. “Control of Listeria monocytogenes in Processed Meats.” Food Australia 44(8): 370–376.
3. Kornacki, J.L. and J.B. Gurtler, “Incidence and Control of Listeria in Food Processing Facilities,” in Listeria, Listeriosis and Food Safety, 3rd ed., eds. Ryser, E.T. and E.H. Marth (Boca Raton, FL: CRC Press, 2007).
4. Kornacki, J.L. 2014. “An Environmental Sampling Approach to Product Risk Assessment.” Food Safety Magazine 20(1).
5. Thimothe, J., et al. 2004. “Tracking of Listeria monocytogenes in Smoked Fish Processing Plants.” J Food Prot 67(2): 328–341.
6. Kornacki, J.L. 2014. “Airborne Contamination: A Microbiologist’s Perspective." Food Safety Magazine 20(3).
7. Kornacki, J.L. 2018. “Whole Genome Sequencing: When and Where Should It Be Used (In Your Plant)?” Presentation at 2nd Annual Kornacki Microbiology Solutions and ClorDiSys Solutions – Gaylord Hotel, Grapevine, TX. February 25–28.
8. Eifert, J.D. and F.M. Arritt. 2002. “Evaluating Environmental Sampling Data and Sampling Plans.” Dairy Food Environ Sanit 22: 333–339.
9. Kornacki, J.L., “Processing Plant Investigations: Practical Approaches to Determining Sources of Persistent Bacterial Strains in the Industrial Food Processing Environment,” in The Microbiological Safety of Low Water Activity Foods and Spices, eds. Gurtler, J.B., J.L. Kornacki, and M.P. Doyle (New York: Springer, 2014).
10. Chen, Y.H., et al. 2009. “Control of Salmonella in Low-Moisture Foods II: Hygiene Practices to Minimize Salmonella Contamination and Growth.” Food Prot Trends 29: 435–445.
Jeffrey L. Kornacki, Ph.D., is president of Kornacki Microbiology Solutions Inc. in Madison, WI. He has performed in-factory microbiological investigations, risk assessments, and food safety-related inspections for 31 years and has made over 850 visits to processing facilities in a variety of capacities with different organizations. He is on the editorial advisory board of Food Safety Magazine.
